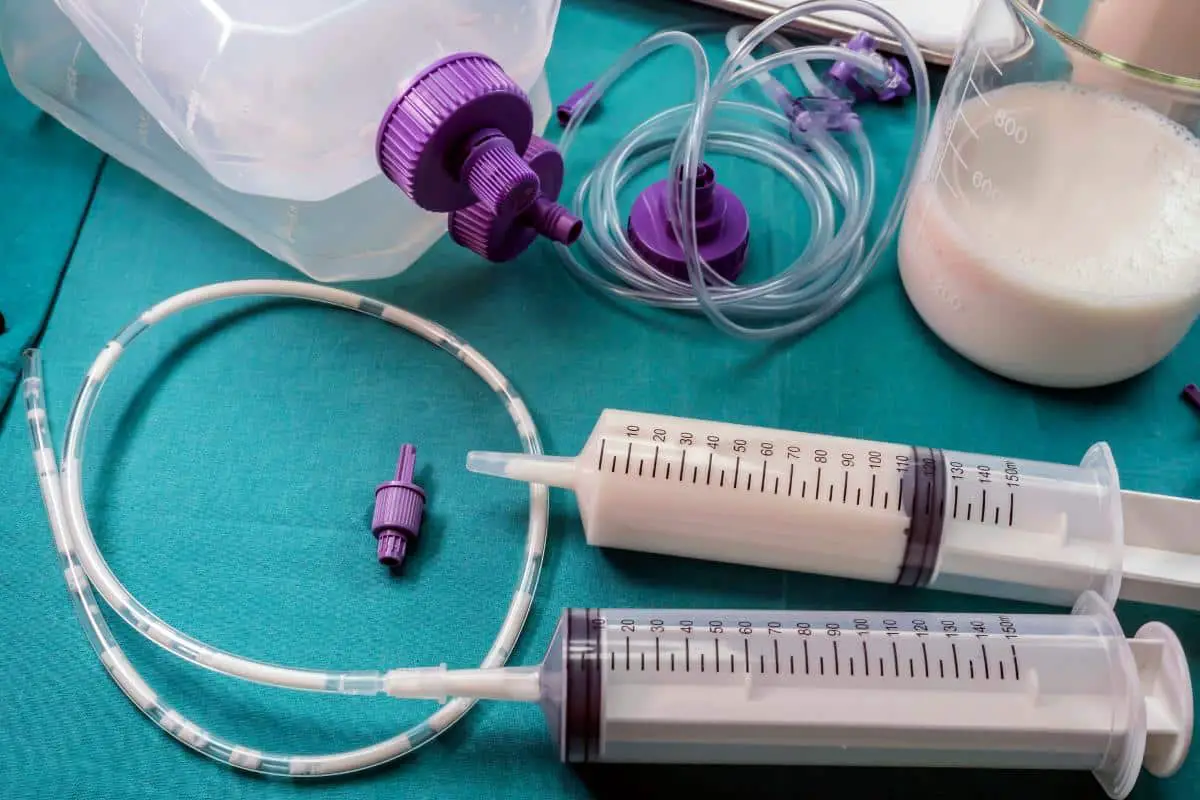
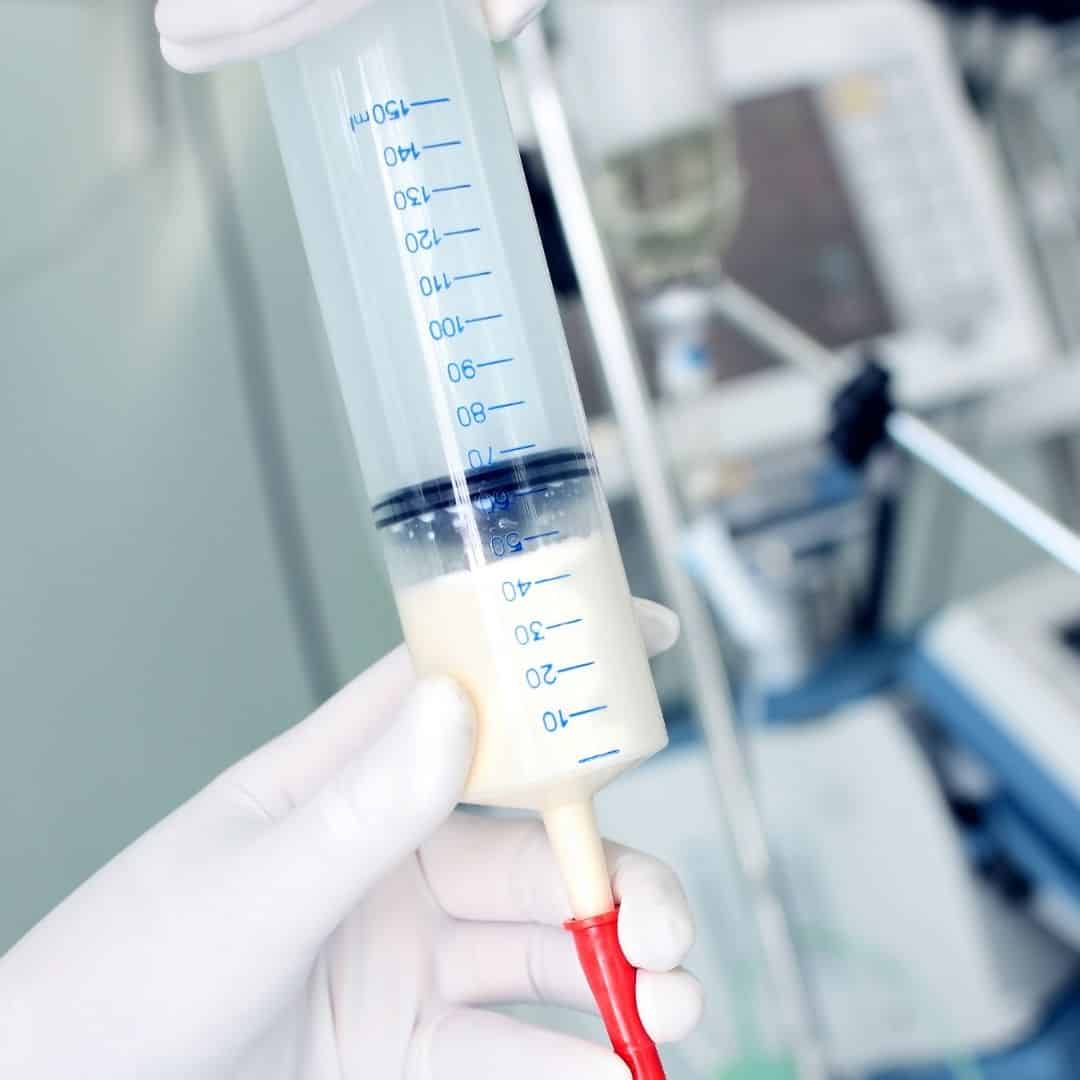
Gastroparesis symptoms can significantly decrease quality of life for older adults. While many cases are able to be managed through diet adjustments, some may require feeding tubes.
What is Gastroparesis?
Gastroparesis is delayed stomach emptying without the presence of a blockage. This can result in life impacting side effects.
Symptoms of gastroparesis include (1):
- Nausea
- Vomiting
- Early satiety: fullness after a small amount of food
- Postprandial fullness: feeling of excess fullness
- Bloating
- Upper abdominal pain
- GERD: gastroesophageal reflux disease
It most commonly has an unknown cause, however can be from surgery, infection, or related to diabetes (2).
Consequences
Gastroparesis can lead to inadequate nutritional intake due to people limiting consumption to avoid symptoms.
Poor intake can lead to malnutrition, unintentional weight loss, muscle breakdown, generalized weakness, and increased falls.
This can all then lead to declined quality of life, resulting in anxiety and depression (3).

Feeding Tube for Gastroparesis
In severe cases of gastroparesis, enteral nutrition may be necessary. Providing nutrition through a feeding tube can ensure proper nutrients are being received.
Being unable to tolerate a liquid diet is predictive that adequate oral intake may not be feasible. In this case tube feeding may be necessary to meet nutritional needs (4).
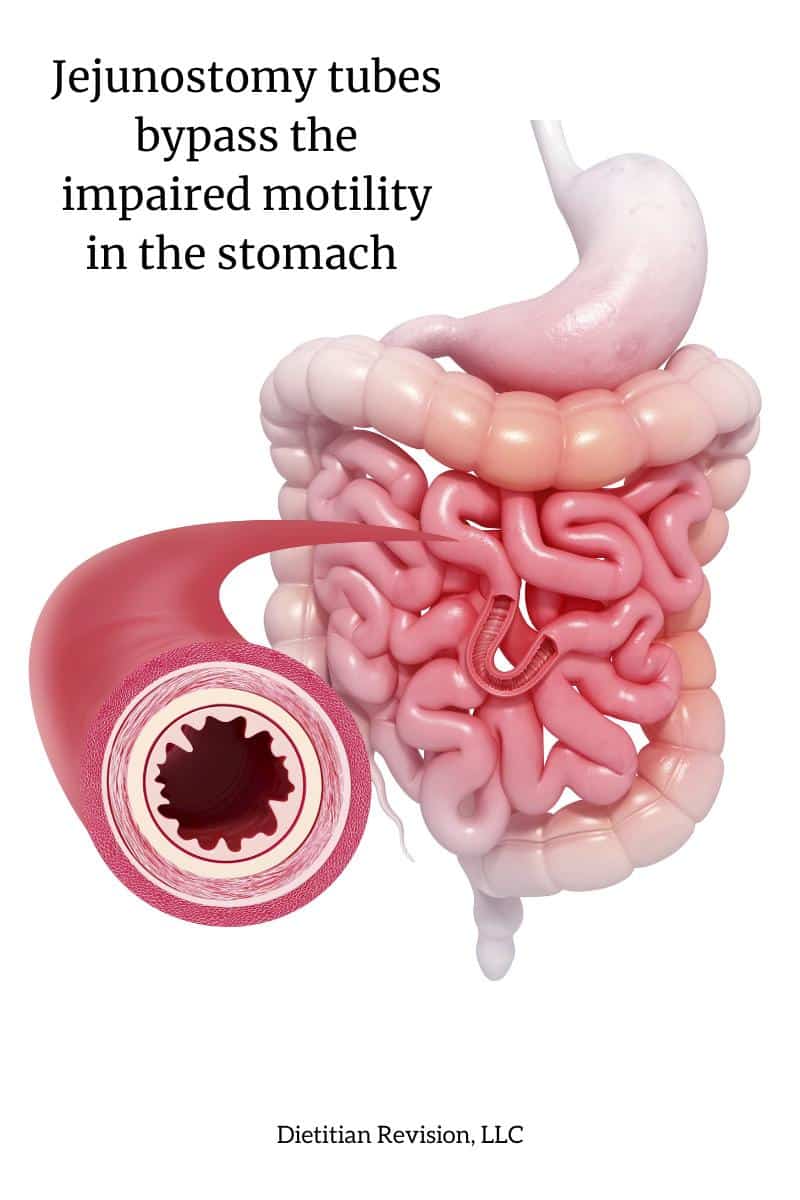
A jejunostomy tube would be placed. This is a feeding tube placed into the small intestine.
This bypasses food going into the stomach, where the motility is impaired. Instead the tube feeding flows right into the jejunum (small intestine).
There are also PEG-J (percutaneous endoscopic gastrostomy jejunostomy) tubes which have a tube that goes to the stomach and a smaller one inside going into the small intestine.
Feeding is provided through the J-port to bypass the stomach and the G-port may be used for venting, suction, or possibly medications.
A nasojejunal tube (a tube going through the nose and down into the small intestine) may be trialed first to ensure tolerance before placing a permanent tube (5).
Benefits
Jejunal feeding tubes for gastroparesis certainly have benefits, including (6):
- Maintained nutritional status
- Relief of gastroparesis symptoms
- Decreased hospital readmissions
- Improved blood sugar control
Improving gastroparesis symptoms, especially pain and nausea, can positively impact quality of life.
Complications
Feeding tubes are not without potential complications, including (7):
- Infection
- Tube dislodgement
- Migration of the tube into the stomach
- Pain
- Diarrhea
Some are less common, however more severe such as (8):
- Bowel perforation
- Major bleeding
- Fistula: an abnormal connection between body parts
- Twisting or knotting of the intestines
- Small bowel obstruction
Practical Takeaways
Gastroparesis can significantly impact quality of life for older adults.
Severe cases may need to be managed with a feeding tube, when an oral diet is unable to be tolerated. For some this may be the only option to maintain proper nutrition.